Introduction to the Healthcare Crisis
Health is a fundamental human right, which is currently in danger on a national and international scale due to the healthcare crisis (WHO, 1966). The healthcare crisis is the massive rise in costs coupled with a failure of the system to provide care to minority groups (PubMed, 2022). Even with federal and state health insurance programs like Medicare and Medicaid striving to make healthcare affordable for those in need of care or financial aid, medical costs have been rising for decades. This is due to several contributing factors, such as unexpectedly high Medicare expenditures, expansion of hospital expenses, and changes in medical care, including increased use of technology, medications, and conservative approaches to treatment (PBS, 2022).
The unaffordability of healthcare is continuing to rise beyond its already extortionate prices. People face hits from increasing health insurance fees, medical bills, and prescription costs – even with insurance coverage, these fees are often crippling (U.S. Census, 2020). A quick visit to the hospital with appendicitis can cost around $5000 (NBC, 2020). Unexpected medical bills were ranked 2nd in the U.S.’s top ‘cost of living anxieties’ in 2022 (Kaiser Family Foundation, 2022).
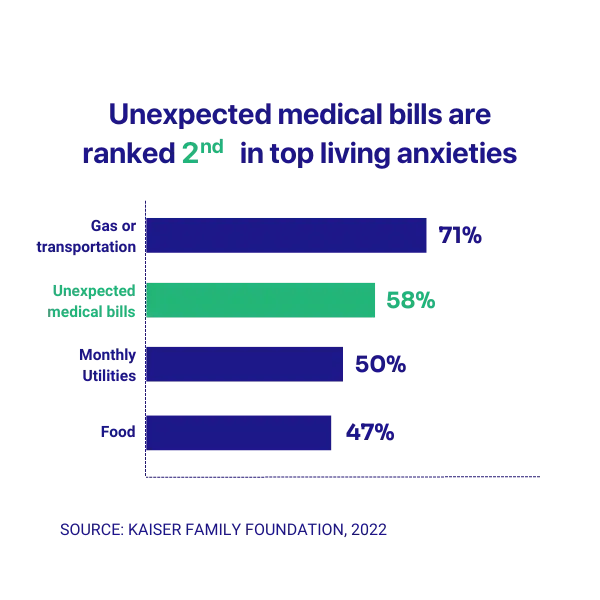
The issue is only expected to become more pressing as there is a rise in employers offering high insurance deductible plans with deductibles increasing, making healthcare less accessible to people who would only be able to pay lower deductibles and wouldn’t be able to afford to pay the higher deductibles (JP Morgan, 2021). In the U.S., the affordability of healthcare is a widely felt issue as the nation struggles with social inequality, reproductive health, and mental illness. The impacts of unaffordable healthcare have strong intersections with race and gender and are a manifestation of systemic oppression.
Racial Gap in Access to Healthcare
One of the significant issues associated with the healthcare crisis is the racial gap in access. Across the U.S., millions of people live without health insurance at any given point in the year. Black, Indigenous, and people of color (“BIPOC”) are overrepresented in this group (U.S. Census, 2020). In 2020, 28 million U.S. citizens did not have health insurance, with Hispanics having the highest uninsured rate (18.3%), followed by Blacks (10.4%) and Asians (5.9%) (U.S. Census, 2020). This overrepresentation means that BIPOC people are less likely to go to routine appointments and put off treatment until the last minute—sometimes too late—because they cannot afford the care they need.
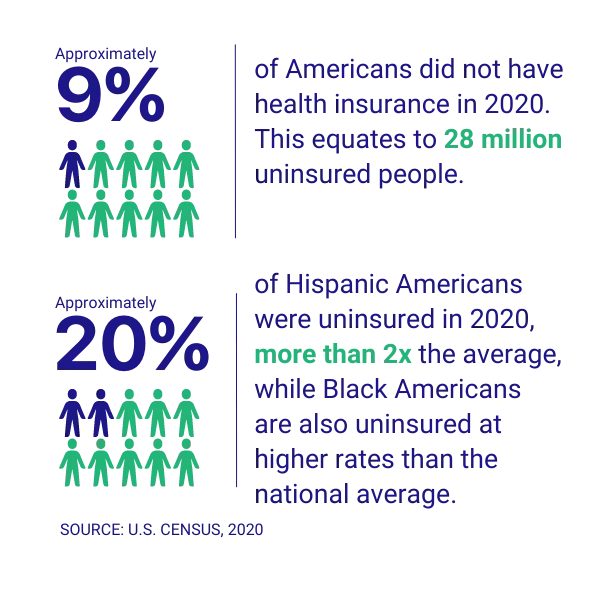
Access to healthcare is also poorer in areas of lower economic status, typically home to BIPOC communities. This disproportionate burden leads to various issues, including the life expectancy of Black Americans being four years lower than White Americans (CDC, 2022). Causes for this access gap include factors beyond affordability, including a lack of diversity in healthcare staff and language barriers that create distrust and inaccessibility of health services. Medical staff are predominantly white, and medical textbooks use white bodies, which leads to issues where doctors do not understand the problems that BIPOC people are facing because they do not understand their bodies (Grady, 2001). Language and cultural barriers also prevent these groups from getting the care they need, as the system makes it more difficult for them to advocate for themselves.
Gender Gap in Access to Healthcare
Women and girls also face extreme inequality in healthcare. Gender inequality in healthcare takes many forms, including underfunded research on the female body, limitations on reproductive rights, and underdiagnoses of fatal conditions. Medical research into patient experience has found that doctors often view men with chronic pain as ‘brave’ or ‘stoic’ but women with chronic pain as ‘emotional’ or ‘hysterical’ (Samulowitz et al., 2018). Much like racial inequality, this is because of a lack of diversity in staff, especially in decision-making positions. Male-dominated boards amplify prejudice and bias toward women, which prevents access to proper care. Women are not believed; they are not advocated for, and they are left behind.
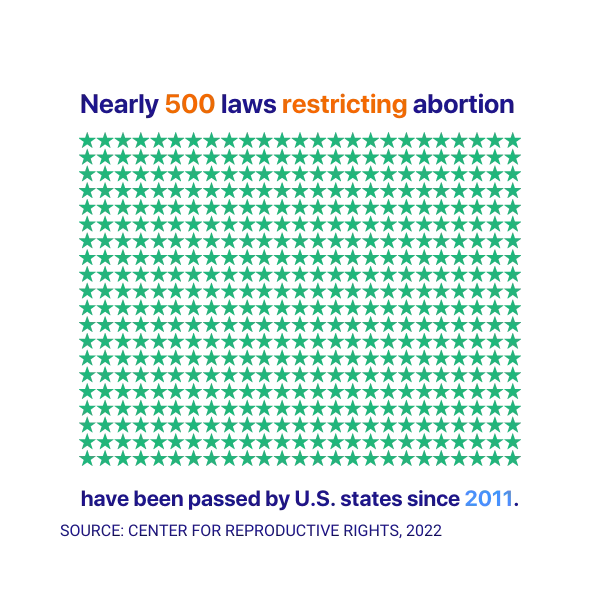
Additionally, with the reversal of Roe vs. Wade, access to safe abortions has and will become less accessible (WHO, 2022). Since 2011 nearly 500 laws restricting abortion access have been passed by U.S states (Center for Reproductive Rights, 2022). The reversal of these laws places a disproportionate and harmful burden on women when they receive healthcare treatment. This burden is especially true for women of lower socioeconomic status who cannot afford to support an unwanted pregnancy, pay medical bills associated with a child born ill, or go to other states and countries to get an abortion.
Women of color also face an unequal risk when bearing children compared to white women. The maternal mortality ratio (MMR) indicates that Black women are three times more likely to die giving birth than their White counterparts. American Indian and Alaskan Native women also fare worse, doubling the MMR of White women (MHTF, 2022). The variance in MMR is attributed to medical staff being predominantly white; language and cultural barriers caused by lack of diversity prevent easily solvable issues from being picked up on until labor. When aiming to fix the gender gap in access to healthcare, we must also prioritize women who are disproportionately affected, specifically women of color and women of lower socioeconomic status.
Barriers to Mental Health Services

The disparity in access is also prevalent in mental healthcare, where people face many barriers. Of the adults that struggle with mental illness, only 45% receive mental health treatment (JP Morgan 2021, NIMH 2022). Mental health access is expensive, making it unaffordable for many people who need care, which disproportionately affects minority groups who have less access to insurance coverage. Services are also not always available, as there are long waiting lists for treatment. Lack of availability prevents people from getting the care they need when they need it, and when the services are finally available, it is sometimes too late, or people need a higher level of care.
The mental health system is also structured to focus on mental health emergencies instead of preventative care. If the system focused on preventing mental health crises, many issues would not become emergencies. Since over half of the adults who struggle with mental illness do not receive treatment, they face unhealthy conditions that could be prevented. Nearly 800,000 people die by suicide each year, roughly one death every 40 seconds, making suicide the second leading cause of death worldwide for people aged 15-24 (Deloitte, 2022). These deaths are preventable, yet there are services that could make a difference, but affordability, approachability, and availability in the healthcare system prevent people from getting the help they need (Coombs, 2021).
Healthcare and the Climate Crisis
Climate change and environmental issues amplify the issues surrounding the healthcare crisis. WHO estimates that over 13 million annual deaths globally are due to avoidable environmental causes, including the climate crisis (WHO, 2022). Various cause-and-effect relationships exist between climate change and health issues, including increased respiratory illnesses from pollution, heat-related health problems from increasing heat events, and water and vector-borne illnesses from reduced food and water quality (EPA, 2022). Many people are at higher risk of these climate-related health issues based on exposure, sensitivity, and ability to adapt (EPA, 2022). Women, BIPOC communities, and lower-income groups face a greater risk of these health issues, which further exacerbate the healthcare access gap, as these people already often cannot afford healthcare services and are in areas of poor accessibility.
Furthermore, the climate crisis also stresses the entire healthcare system: the increased frequency, intensity, and variability of natural disasters and their downstream effects challenge healthcare systems’ infrastructure, supply chain, and workforce (Deloitte, 2022). The stress on the healthcare structure caused by climate change will further decrease access to adequate healthcare, as people will not have the facilities to get the help they need. Climate deaths will only get worse if we do not address climate change.
No one should ever be in a position where they cannot afford to take care of their health or where they do not feel comfortable getting the help they need. These pressing issues will only worsen unless we make structural changes to the healthcare system.
Introduction to Affordable Healthcare Solutions
People should not have to choose between utility bills or medical bills. We can make healthcare more affordable and reduce the race and gender inequality experienced within the healthcare system. Making healthcare affordable is a social, economic, and public health imperative.
One of the United Nations’ 17 Sustainable Development Goals (the UN SDGs) aims to “ensure healthy lives and promote wellbeing for all, at all ages.” SDG 3 Good Health and Wellbeing works to solve many issues surrounding the healthcare crisis by 2030, including its intersection with race, gender, mental health, and climate change. The goal is comprehensive; however, it will take a culmination of government and industry cooperation to address the healthcare crisis and make healthcare affordable and accessible for all. The UN outlines a range of targets as a guideline to achieve global health. One of the issues that the UN aims to address is the mental health crisis. To help this issue, the UN proposes that governments reduce one-third of premature mortality from non-communicable diseases through prevention and treatment and promote mental health and wellbeing by 2030, improving affordability and access to mental healthcare.
The UN also wants to address the gender disparity in access to healthcare. To accomplish this goal, they encourage governments to ensure universal access to sexual and reproductive healthcare services to reduce unwanted pregnancies. Access to sexual and reproductive healthcare is also a target of SDG 5 Gender Equality. To help with the affordability of healthcare and lessen the racial gap in access, the UN is calling for governments to achieve universal health coverage, including financial risk protection, access to quality essential healthcare services, and access to safe, effective, quality, and affordable essential medicines and vaccines for all. Addressing the impact of climate change on the healthcare crisis is also a priority in the SDGs. One target supporting this cause is for governments to improve the environmental harms that cause health issues by 2030 by substantially reducing the number of deaths and illnesses from hazardous chemicals and air, water, and soil pollution and contamination. In order to reach these targets, we must reform insurance, implement national policies, and improve technology. These goals set ambitious targets that would help reduce many of the issues surrounding the healthcare crisis, but we must take action to ensure that they are met.
In action, solutions to the U.S. healthcare crisis take three forms: renewing and reforming legislature, investing in telehealth, and improving occupational health regulation. Addressing healthcare legislation will ensure that treatment is consistent and access is better regulated to ensure that people can get the care they need regardless of their race, gender, or socioeconomic status. Implementing national policies and infrastructure to provide affordable healthcare is required, such as the Affordable Healthcare Act and the Prescription Drug Legislation. Additionally, by incorporating telehealth and telemedicine, healthcare companies will have a greater reach, allowing treatment to be more easily accessible for patients that may otherwise face several barriers. Increasing and improving occupational health regulation will help promote and maintain workers’ physical, mental, and social wellbeing. This improvement will ensure that people can improve all aspects of their health, specifically mental health, to ensure that people get the treatment they need. People can help implement these solutions by investing in companies tackling these issues and paving the way for a more sustainable future.
NGO Spotlight
Non-governmental organizations also play a prominent role in securing access to affordable healthcare. To achieve affordable and equitable care for all, it will take a global movement and collaboration of players to come together and provide resources and technical expertise that will advance this vision of fair access to healthcare. To create lasting change, FLIT Invest has partnered with Medic who share this joint vision.

Medic serves as technical steward and core contributor of the Community Health Toolkit (CHT), a global public good that supports community health workers (CHWs) as they deliver care in reimagined health systems.
The CHT includes a collection of open-source software frameworks and applications, with resources to help partners design and deploy digital tools (“apps”) for care teams. Medic partners with local and national governments, implementers, public and private technology partners, researchers, and local communities to develop people-focused, sustainable solutions that meet health, wellbeing, and development needs. For millions of households, interactions with CHT-supported CHWs may be the only moments when their care is recorded and reported into the formal health system — making care and care work visible.

Medic and the CHT have supported more than 120 digital community health initiatives since their inception, bringing learnings from each to the open access community of practice. Digital health apps built using the CHT are actively deployed in 15 countries in Africa and Asia and are used by 40,000+ health workers who have supported 90+ million caring activities since tracking of this metric began in 2014. Last year alone, health workers completed over 22 million caring activities for families living at the last mile. To learn more about Medic, please visit their website.
FLIT Invest Affordable Healthcare Portfolio
FLIT Affordable Healthcare portfolios contain over 35 companies representing progress towards affordable healthcare and reflecting your personal goals.
The 3 main metrics used at FLIT to measure companies’ progress in Affordable Healthcare are:
- Number of human lives improved
- Medical costs covered ($)
- Prescriptions provided

Investment Rationale
The managed care industry is best positioned to effectively temper runaway healthcare spending in partnership with the U.S. Government and drive structural changes to the existing delivery system in America (Fidelity, 2021). Value-Based Care brought significant changes to the industry, focusing on the quality of care and is driven by advancements in technology and analytics which enabled providers to move towards whole-person care. Significant changes in consumer behavior (such as telemedicine) are driving tech-enabled players’ revenues. Patients increasingly favor providers offering greater convenience, high-quality service, and lower costs.
Company Spotlight
Agilon Health (AGL)
Agilon Health’s vision is to transform the future of health care in 100+ communities across the country by empowering exceptional patient-physician relationships, and they are working towards this vision by empowering physicians, unlocking value-based care, transforming communities, and ensuring that the company is built by people who care about the issue. $101 million has been invested back into physician partners and healthcare delivery in their communities, and 43% of Agilon physician partner practice locations reside in federally designated, underserved communities, which allows people who may not otherwise have access to adequate healthcare to get the help and treatment that they need, lessening the gaps.
Oak Street Health (OSH)
Oak Street Health’s mission is to build a primary care delivery platform for Medicare beneficiaries that addresses two key issues: rising costs and poor quality of healthcare. They advocate preventative care, compassionate patient-doctor relationships, and insurance education. OSH services have cared for over 150,000 patients across 20 states; approximately half of their patients are BIPOC. On top of this, the company ranks in the top 10 of Russell 1000 companies for racial justice and 2nd best for healthcare specifically (As You Sow, 2021).
Benefits of Expert Curation on Affordable Healthcare Investing

Our team at FLIT has researched hundreds of investment funds and companies, and we have curated a portfolio that we believe targets affordable healthcare. These companies cover managed care, value-based care, drug retail and distributors, dental distributors, tech-enabled providers, and facilities – each service or product helps to advance affordable healthcare. We provide users with transparent data on the sustainability practices of each company to ensure an investment aligns with your values. We strongly believe that this approach to investment is essential for our future and profitable.
Your investments have the power to shape the future. Do you believe that healthcare should be accessible and affordable? Do you believe more needs to happen in order to achieve gender and racial justice within healthcare? If so, investing in Affordable Healthcare might be right for you. Monumental progress is needed in the make healthcare accessible and affordable for all, and if companies will not change their practices or policies, then it is up to us investors to band together and vote with our dollars. We have the power to shape the future, we have the power to drive systemic change. Invest today for Affordable Healthcare with FLIT – sign up today and start investing for a better future.
Footnote 1: Content is for informational and educational purposes only. Any views, strategies or products discussed may not be appropriate for all individuals and are subject to risks. Investors may get back less than they invested, and past performance is not a reliable indicator of future results. The information contained herein should not be construed as, and may not be used in connection with, an offer to sell, or a solicitation of an offer to buy or hold, an interest in any security or investment product. Investors should carefully consider the investment objectives and risks as well as charges and expenses of a mutual fund or ETF before investing.



